Uterine Fibroid Morcellation Cancer Risk May Be Overstated: Gynecologists
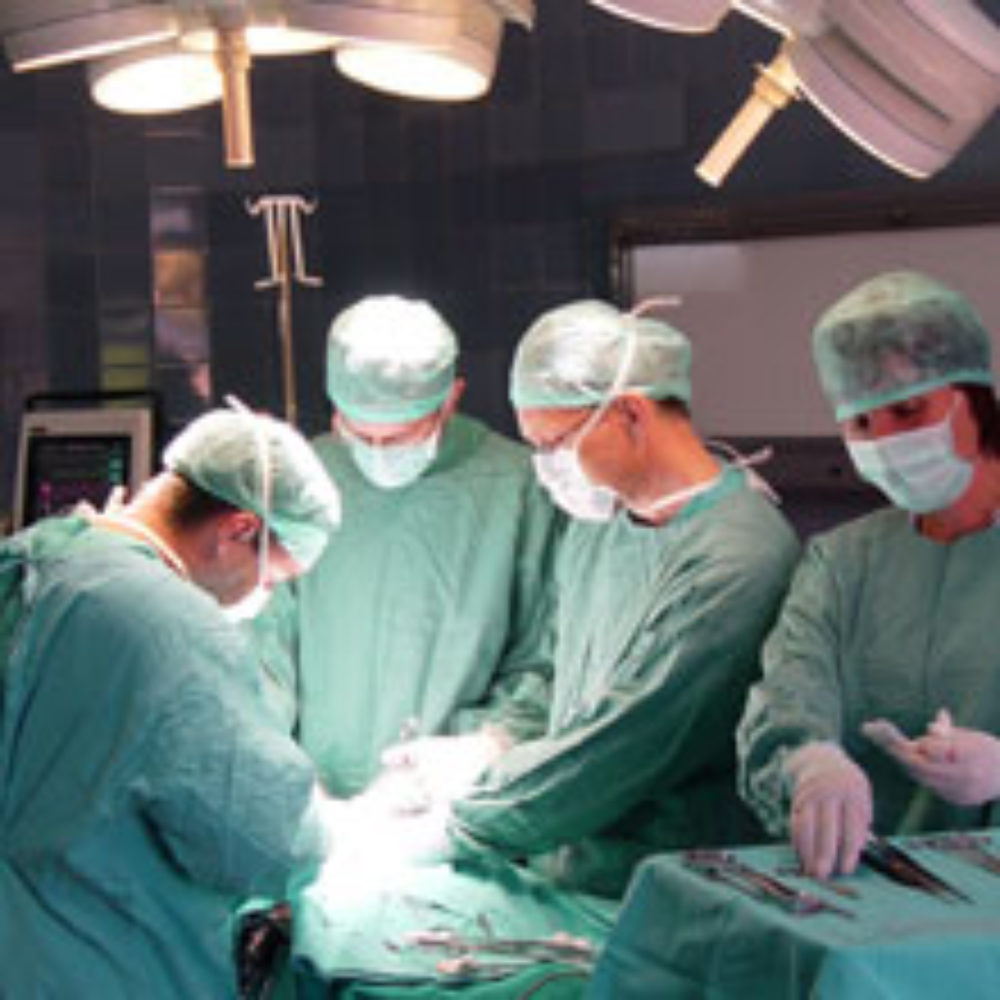
As a growing number of hospitals are announcing that they will no longer perform hysterectomies or uterine fibroid surgery with morcellators, due to the risk of spreading cancer, two major gynecological organizations have issued policies defending uterine fibroid morcellation, claiming that the cancer risk must be weighed against the benefits provided by minimally invasive surgery.
The American College of Obstetricians and Gynecologists (ACOG) and the AAGL, formerly the American Association of Gynecologic Laparoscopists, issued policy guidelines for members, which indicate that laparoscopic hysterectomies using power morcellation are generally safe, despite recent warnings issued by the FDA urging doctors to avoid use of morcellators due to the risk that the devices may spread unsuspected sarcoma for some women.
Morcellation involves the use of a hand-held medical device during laparoscopic or robotic surgery to cut up the uterus or fibroid tumors, and remove the tissue through a small incision in the abdomen. This allows women to undergo a minimally invasive procedure, with reduced recovery times and less risk of infections and other complications.

Learn More About
Power morcellators used during a laparoscopic hysterectomy or uterine fibroid surgery may cause the spread of aggressive cancer.
Learn More About this Lawsuit SEE IF YOU QUALIFY FOR COMPENSATIONOn April 17, the FDA issued a warning to health care providers that indicated about 1 out of every 350 women who undergo these procedures may have unsuspected sarcoma in their uterus, and morcellation may spread the cancerous tissue throughout the abdomen, potentially reducing the chances for long-term survival. Because there is no reliable way for doctors to detect the uterine cancer prior to the surgery, the FDA urged doctors to avoid uterine fibroid morcellation and to consider alternate surgical techniques.
According to the policy guidelines issued by the ACOG and AAGL, the overall risk of deadly cancer being spread is rare and the groups indicate that doctors should not abandon morcellation for uterine fibroids.
“It is well established that minimally invasive surgical techniques for hysterectomy and myomectony reduce the risk of intraoperative and postoperative morbidity and mortality,” ACOG wrote in its policy guidelines (PDF). “Without power morcellation, some patients may be ineligible for minimally invasive gynecologic surgery.”
The organization said it was impossible to conduct a surgical procedure without risk, and notes that there could be ways to make the procedures safer.
While the FDA indicated that about 1 out of every 350 women who undergo a laparoscopic hysterectomy or myomectomy may have unsuspected sarcoma, and 1 out of every 498 women who undergo the procedure has leiomyosarcoma contained within the uterus, the ACOG has cast doubt on the usefulness of the FDA’s numbers.
“Various sources cite estimates of occult uterine sarcoma, ranging from 2:1000 to 1:350. While these incidence numbers are within the same statistical range, they have questionable applicability because of the rarity of the disease, the small sample size, age variability, and lack of age stratification,” ACOG notes. “In addition, it is important to note that none of these estimates take into consideration the number of uterine sarcomas that were morcellated.”
According to AAGL, nearly half of the 400,000 inpatient-based hysterectomies performed every year in the U.S. include power morcellation. However, in the AAGL policy guidelines (PDF), the organization acknowledges that there are serious concerns, noting that using a morcellator prevents comprehensive evaluation of the uterine fibroid specimen.
“Additionally, dissemination of tumor or uterine fragments, either benign or malignant, throughout the intraperitoneal cavity may necessitate further surgical interventions or other treatment and may worsen prognosis,” AAGL admitted. “The possibility of this complication may have been previously underestimated.”
Both organizations called for further investigations into the effectiveness of “specimen bags,” which could potentially contain uterine fibroid tissue. They also advised against using power morcellation where malignant uterine fibroids were suspected or among women with a higher risk of cancer, such as postmenopausal women.
Following the FDA warnings, many hospitals have already released statements indicating that they will no longer be performing laparoscopic hysterectomy or uterine fibroid surgery with morcellation.
Johnson & Johnson’s Ethicon subsidiary, which was the leading manufacturer of power morcellators, also announced late last month that it was halting sales and distribution of power morcellators until the FDA and medical communities can determine the correct course of action regarding the devices.
The FDA has indicated that it will convene a public meeting of the Obstetrics and Gynecological Medical Device Advisory Committee to discuss the clinical role of laparoscopic morcellators in treatment of uterine fibroids and whether surgical techniques or the use of accessories like tissue collection bags may make the devices safer. The FDA advisory committee will also review whether a “boxed warning” should be placed on all laparoscopic power morcellators regarding the risk of spreading cancer.
Lawsuits Over Uterine Fibroid Surgery Morcellation
As women and families learn that cases of aggressive uterine cancers diagnosed following a laparoscopic hysterectomy or myomectomy may have been caused by morcellation, questions are being raised about why adequate warnings were not provided and whether manufacturers failed to make the devices as safe as they could have been.
A number of uterine fibroid morcellation lawsuits are now being pursued on behalf of individuals who had leiomyosarcoma, endometrial stromal sarcoma or other cancers spread during the procedures.
Plaintiffs allege that as they are currently designed, power morcellators are unreasonably dangerous.
In addition, women claim that they may have avoided spreading cancer throughout their body if information about the risk had been provided to the medical community, since a number of alternative treatment options are available for women with symptomatic uterine fibroids, including traditional surgical hyesterectomy performed vaginally or abdominally, catheter-based blocking of the uterine artery, high-intensity focused ultrasound, drug therapy and laparoscopic hysterectomy or myomectomy without use of morcellation.
Get more articles like this sent directly to your inbox.
"*" indicates required fields
1 Comments





BeverlyJuly 17, 2014 at 1:08 pm
I had fibroid tumors, after having 4/5 transfusions I had surgery a vaginal hysterectomy. My ovaries were not taken. Within a week I had my feet and ankles swell up big as elephants feet. I went to E.R they said I had Cellulites, that was 2011. I have suffered with this swelling in my ankles, sometimes both feet since. I HAVE ALL DOCUMENTATION, Pictures of every time my ankles would swell, and[Show More]I had fibroid tumors, after having 4/5 transfusions I had surgery a vaginal hysterectomy. My ovaries were not taken. Within a week I had my feet and ankles swell up big as elephants feet. I went to E.R they said I had Cellulites, that was 2011. I have suffered with this swelling in my ankles, sometimes both feet since. I HAVE ALL DOCUMENTATION, Pictures of every time my ankles would swell, and of all E.R. visits. I have weakness in ankles due to all the swelling I've been through. Its crazy I have even been put on crutches when ankles feet swell. I think they caused my problem, I was fine till that surgery.