Laparoscopic Hysterectomy Leiomyosarcoma Risks Balanced by Benefits Over Abdominal Surgery: Study
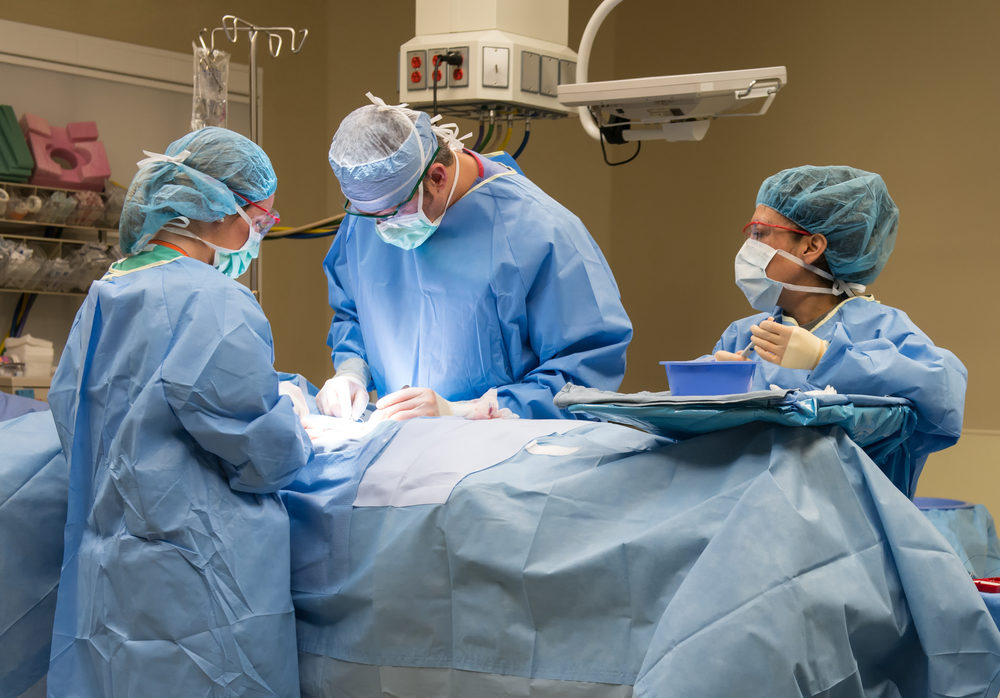
As concerns continue to mount within the medical community about the risk of spreading leiomyosarcoma during a laparoscopic hysterectomy with morcellation, a recent study suggests that the minimally invasive procedures may still be safer than an abdominal hysterectomy when factoring in the risk of infections and other potentially life-threatening problems.
Researchers from the University of North Carolina at Chapel Hill published a study this week in the American Journal of Obstetrics & Gynecology, which found that abdominal surgery to remove uterine fibroids carries a higher risk of complications and death than laparoscopic procedures involving the use of morcellators.
In recent months, the medical community has largely moved away from the use of power morcellators, which are able to cut up and remove tissue through a small abdominal incision. Since many women may have unsuspected sarcoma contained within their uterus, which doctors are unable to diagnose before the procedure, most experts now believe that the risk that morcellators may disseminate leiomyosarcoma or other uterine cancers is too great to justify the laparoscopic procedures.

Learn More About
Power morcellators used during a laparoscopic hysterectomy or uterine fibroid surgery may cause the spread of aggressive cancer.
Learn More About this Lawsuit SEE IF YOU QUALIFY FOR COMPENSATIONIn this latest study, researchers used a hypothetical model of 100,000 premenopausal women who underwent hysterectomies for uterine fibroid removal over a period of five years. It predicts that there would be 98 deaths per 100,000 women among those who underwent laparoscopic hysterectomy, but that there would be 103 per 100,000 women who died if they got an abdominal hysterectomy.
Researchers found there would be more deaths due to leiomyoscarcoma among women who underwent power morcellation, but that abdominal hysterectomies would result in more wound infections, needs for blood transfusions, incision hernias, and other risks.
“The risk of leiomyosarcoma morcellation is balanced by procedure-related complications that are associated with laparotomy, including death,” the researchers concluded. “This analysis provides patients and surgeons with estimates of risk and benefit on which patient-centered decisions can be made.”
Laparoscopic Hysterectomy Cancer Risks
In April 2014, the FDA issued a statement about the risk of power morcellators spreading uterine cancer, indicating that an estimated one out of every 350 women undergoing a hysterectomy or myomectomy may have unsuspected uterine sarcoma.
Following a safety review, the FDA announced in November that new “black box” warnings will be required for all morcellators, warning about the risk of spreading cancer and contraindicating the use of the devices on most likely patients.
While it is rare for women to have unsuspected leiomyosarcoma or other cancers, spreading the aggressive cells throughout the abdomen is a virtual death sentence for women, greatly reducing the chances for long-term survival and rapidly diminishing their overall quality of life. As a result, the medical community has been pulling away from the use of morcellation for uterine fibroid removal and a number of major insurance companies now say they will not cover the procedure, or will only do so under strict circumstances. In addition, a number of hospitals and health care networks are also eschewing the practice.
Manufacturers of the devices now face a growing number of morcellator cancer lawsuits, alleging that the devices were sold without adequate warnings about the risk of leiomyosarcoma, endometrial stromal sarcoma or other uterine cancers.
Plaintiffs allege that the rapid spread of cancers may have been avoided if any number of different alternative treatment options available for women with symptomatic uterine fibroids had been used, including traditional surgical hysterectomy performed vaginally or abdominally, catheter-based blocking of the uterine artery, high-intensity focused ultrasound, drug therapy and laparoscopic hysterectomy or myomectomy without use of morcellation.
Get more articles like this sent directly to your inbox.
"*" indicates required fields





0 Comments