Morcellation Collection Bag May Reduce Risk of Spreading Cancer: Study
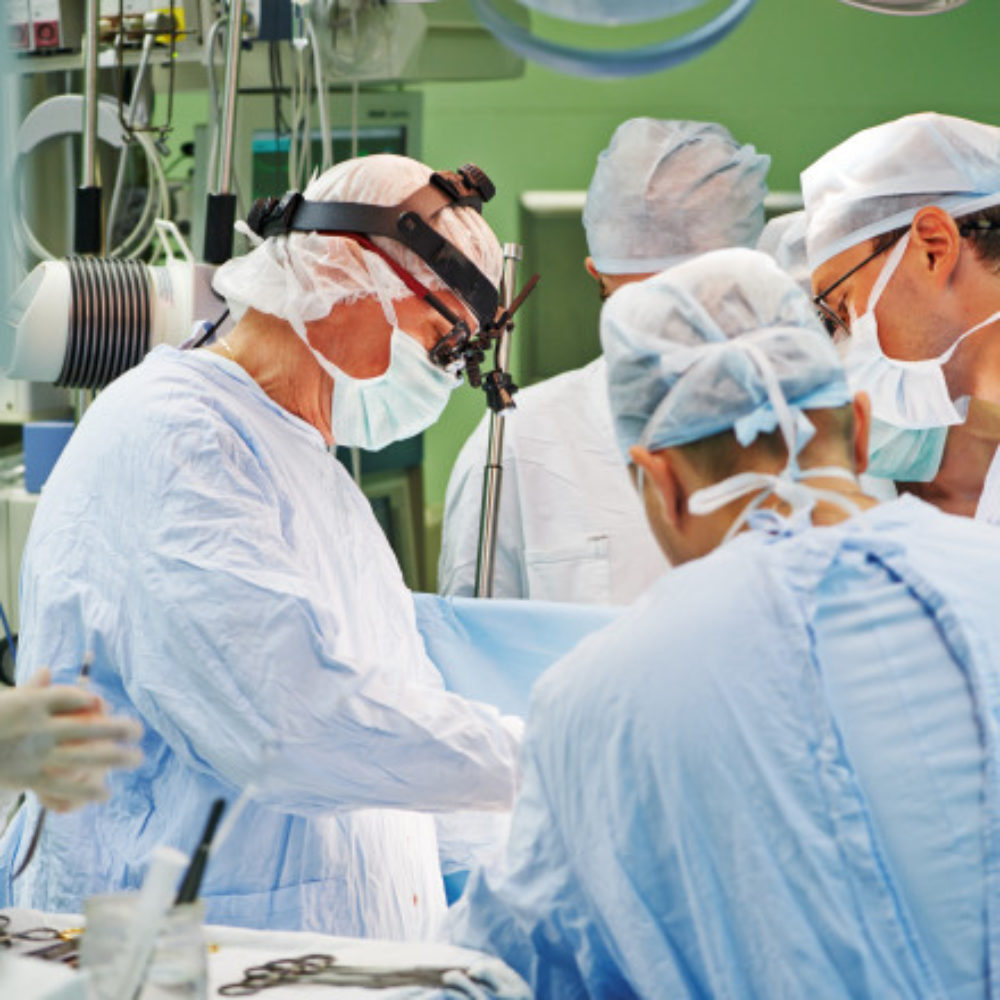
Amid continuing concerns about the spread of cancer associated with morcellation during uterine fibroid surgery, new research suggests that the use of inflated tissue collection bags during a laparoscopic hysterectomy or myomectomy may protect women from the accidental spread of cancerous cells.
In a study published by the medical journal Obstetrics & Gynecology on August 5, researchers from Brigham and Women’s Hospital and the Center for Minimally Invasive Gynecologic Surgery in Massachusetts found that the use of morcellator collection bags may make the minimally invasive procedures safer.
Power morcellators are medical devices that became increasingly popular in recent years, commonly used during a laparoscopic hysterectomy or uterine fibroid removal surgery to allow the doctors to cut up the uterus or fibroid and remove the tissue through a small incision in the abdomen. However, hospitals and doctors have recently begun to abandon the devices following an FDA warning earlier this year, which indicated that power morcellation may spread cancer cells for women with an unsuspected sarcoma prior to the procedure.

Learn More About
Power morcellators used during a laparoscopic hysterectomy or uterine fibroid surgery may cause the spread of aggressive cancer.
Learn More About this Lawsuit SEE IF YOU QUALIFY FOR COMPENSATIONAbout one out of every 350 women who undergo the uterine fibroid surgery may have undiagnosed cancer contained within their uterus. Doctors are unable to diagnose the cancer prior to the surgery, and use of the power morcellator has been linked to the rapid spread of leiomyosarcoma, endometrial stromal sarcoma or other cancers throughout the abdomen, quickly upstaging the cancer and decreasing the chances for long-term survival.
Morcellation collection bags have previously been available, but the accessories were not included with the devices and there has been a lack of evidence that they are effective in collecting tissue spread by power morcellators. In addition, many surgeons did not appreciate the link between power morcellators and cancer, due to a lack of prior warnings provided to the medical community.
When the morcellators grind up the fibroids containing the undiagnosed cancer cells, it can spread them throughout the body cavity, pushing the cancer from undiagnosed and at its lowest level, to its most advanced and deadly stages. The isolation bags, also known as insufflated collection bags, are supposed to catch the debris, keep it contained, and allow it to be easily removed.
Last month, a panel of FDA advisors met and determined that there was no data indicating the bags were safe or effective and that there was no way to conduct power morcellation on uterine fibroids safely.
However, researchers working on this latest study indicate that they looked at data on 73 women who underwent uterine tissue morcellation with the aid of a collection bag at four institutions from January 2013 through April 2014. Doctors maneuvered the uterine fibroids into a 50-by-50-cm bag, insufflated in the peritoneal cavity, and then used the power morcellator within the bag so that it caught the debris and fluids. They said that the median operation time was 114 minutes and 78% of the patients were discharged from the hospital the same day.
“Morcellation within an insufflated isolation bag is a feasible technique,” the researchers concluded. :Methods for morcellating uterine tissue in a contained manner may provide an option to minimize the risks of open power morcellation while preserving the benefits of minimally invasive surgery.”
However, the study was accompanied in the same journal by an editorial by Dr. Charles R. Rardin, of the urogynecology division at Women and Infants’ Hospital in Providence, Rhode Island, who raised some questions about the ease of use and practicality of the isolation bags.
Rardin noted that there are several questions about the plausibility and safety of collection bags, despite the findings of the study. The editorial pointed out that the study relied only on doctors’ visual assessment of whether the bags caught all the debris.
Power Morcellation Falling Out of Favor
Following the FDA’s recommendations to doctors to avoid using power morcellators, a number of hospitals and practices have banned the procedure or put a moratorium in place until the FDA makes some kind of permanent decision on whether the devices can be used or if there needs to be a power morcellator recall.
However, the largest manufacturer of power morcellators, the Johnson & Johnson subsidiary, Ethicon, recently announced a power morcellator recall, indicating that it was getting out of the morcellation business until and unless new technology can make the procedure safer. Prior to the decision, Ethicon manufactured more than 70% of all power morcellators.
Last week, Highmark, Inc. an east coast, Pennsylvania-based health insurance provider, announced that it would no longer cover power morcellation procedures. Highmark also owns the West Penn Allegheny Health System, which means that the procedure will no longer be performed throughout much of Pennsylvania after the first of next month. The company also provides coverage in Delaware and West Virginia, and the insurer indicates that it hopes other hospital systems and health insurance companies will follow suit.
Laparoscopic Hysterectomy Morcellation Lawsuits
As women and families learn that cases of aggressive uterine cancers diagnosed following a laparoscopic hysterectomy or myomectomy may have been caused by morcellation, questions are being raised about why adequate warnings were not provided and whether manufacturers failed to make the devices as safe as they could have been.
A number of laparoscopic hysterectomy morcellation lawsuits are now being pursued on behalf of individuals diagnosed with leiomyosarcoma, endometrial stromal sarcoma or other cancers spread following a hysterectomy or myomectomy performed laparoscopically or through robotic surgery.
Plaintiffs allege that as they were originally designed and sold, power morcellators are unreasonably dangerous. In addition, women claim that they may have avoided spreading cancer throughout their body if information about the risk had been provided to the medical community, since a number of alternative treatment options are available for women with symptomatic uterine fibroids, including traditional surgical hyesterectomy performed vaginally or abdominally, catheter-based blocking of the uterine artery, high-intensity focused ultrasound, drug therapy and laparoscopic hysterectomy or myomectomy without use of morcellation.
Get more articles like this sent directly to your inbox.
"*" indicates required fields





0 Comments