Medication Errors Over Brilinta, Brintellix Name Mix-Ups Lead To FDA Warning

Federal drug regulators are warning about the potential risk of medication errors with Brilinta and Brintellix, which doctors, pharmacists and consumers often mix up up due to the similar names, which may result in adverse health events.
A safety advisory was issued by the FDA on Thursday, warning about the importance of carefully prescribing, filling and using the Brintellix and Brilinta.
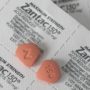
As of June 15, the FDA had received more than 50 reports of medication confusion between the two drugs, which likely only represents a small fraction of the total number of adverse events caused by the confusion. Reports stem from the similarity not only of the name, but also the tablets as well. Both may be dispensed as a yellow tablet at times.

Did You Know?
Millions of Philips CPAP Machines Recalled
Philips DreamStation, CPAP and BiPAP machines sold in recent years may pose a risk of cancer, lung damage and other injuries.
Learn MoreSoftware used to order prescription medications in medical offices and pharmacies add to the risk of medication mistakes. Both names are populated after the first three letters are typed in, making it even easier for medical professions to order the incorrect medication.
However, so far, the FDA says there are no reports of patients ingesting the wrong medication.
Brilinta is an anti-platelet, anti-blood clotting medication that lowers the risk of having another heart attack or dying from heart problems following a heart attack or severe chest pain. The drug keeps the platelets from sticking together, preventing blood clots from forming. The tablets are round and yellow, with a 90 above a T stamped on one side. It is manufactured by Astrazeneca PLC and generated more than $100 million in sales this quarter.
Brintellix is used to treat a serious form of depression known as major depressive disorder (MDD) in adults which affects a chemical in the brain that becomes unbalanced. It is manufactured by Japanese based company, Takeda Pharmaceuticals, which reported $42 million in revenue from Brintellix in the latest quarter. The medication is a selective serotonin reuptake inhibitor (SSRI) and is a tear-shaped tablet stamped with TL on one side and a number that indicates the tablet strength on the other side. It varies in color depending on the strength.
The FDA recommends health care professionals take steps to reduce the risk of mix-up by also including the generic name of the medication and the brand name on the prescription and medication bottle. In this case, the generic name for Brintellix is vortioxetine and the generic name for Brilinta is ticagrelor.
The reason for the prescription should also be added, the FDA suggests. Patients should also double check their prescription to ensure the correct medication has been dispensed.
Medication Mix-Ups
The FDA reviews drug names before they are approved for public use. During the lengthy process the agency compares the drugs name to others on the market and those under FDA review to ensure drug confusion doesn’t occur.
When approving names the FDA creates a list of names that could be confused with the proposed drug. During the process the FDA reviews spelling, pronunciation in different accents and how the name will appear written by hand in different handwriting samples. More than 22 pages are written on guidelines for drug name approval.
The FDA will reject names that confuse consumers. More than 400 proposed drug names are review every year. The FDA rejects about one-third of them. Generic drug names are monitored by the U.S. Adopted names Council.
Similar warnings have been issued in the past about the risk of medication errors from drugs with similar names.
In 2011, the FDA warned about the risk of confusion between the Parkinson’s disease drug Requip and the antipsychotic medication Risperdal, following more than 226 reports of problems where individuals took the wrong drug, including at least five cases that resulted in patients being hospitalized.
The FDA approved a name change for the heartburn drug Kapidex in 2010, after receiving reports of pharmacists confusing it with other drugs, such as the prostate cancer drug Casodex or the morphine-based pain killer Kadian.
A drug safety communication issued in 2013 warned about the risk of confusing Herceptin and Kadcyla, given the similar generic names of trastuzumab and ado-trastuzumab emtansine.
Brilinta Approval Concerns
Brilinta’s approval itself has been a subject of controversy.
The U.S. Department of Justice launched an investigation into previous clinical trials on Brilinta in 2013, after a report identified a number of irregularities in a clinical trial and suggested that reports of heart attacks linked to Brilinta may have been under-reported.
In August 2013, a study published in the International Journal of Cardiology suggested that AstraZeneca may have manipulated data during an 18,000-patient clinical trial to make the drug appear safe when data suggested otherwise.
Among the irregularities was the fact that an independent review of the data found that 46% of all primary endpoint events favoring Brilinta came from just two countries, Poland and Hungary, despite the participation of subjects from numerous other countries. The review also found that heart attacks linked to Brilinta were under-reported in the clinical trial findings.
The trial, known as PLATO, was used to get Brilinta approved for the market in 2011. The company had hoped to make the drug one of its flagship medications, but to date sales have been disappointing.
In October 2013, a study was presented at the European Society of Cardiology, where researchers from the Netherlands warned that a significant number of patients are dropping the drug due to side effects of Brilinta, which include breathlessness and other health problems.
Get more articles like this sent directly to your inbox.
"*" indicates required fields




0 Comments