Smart Infusion Pump Problems Targeted By New ISMP Guidelines For Hospital Use
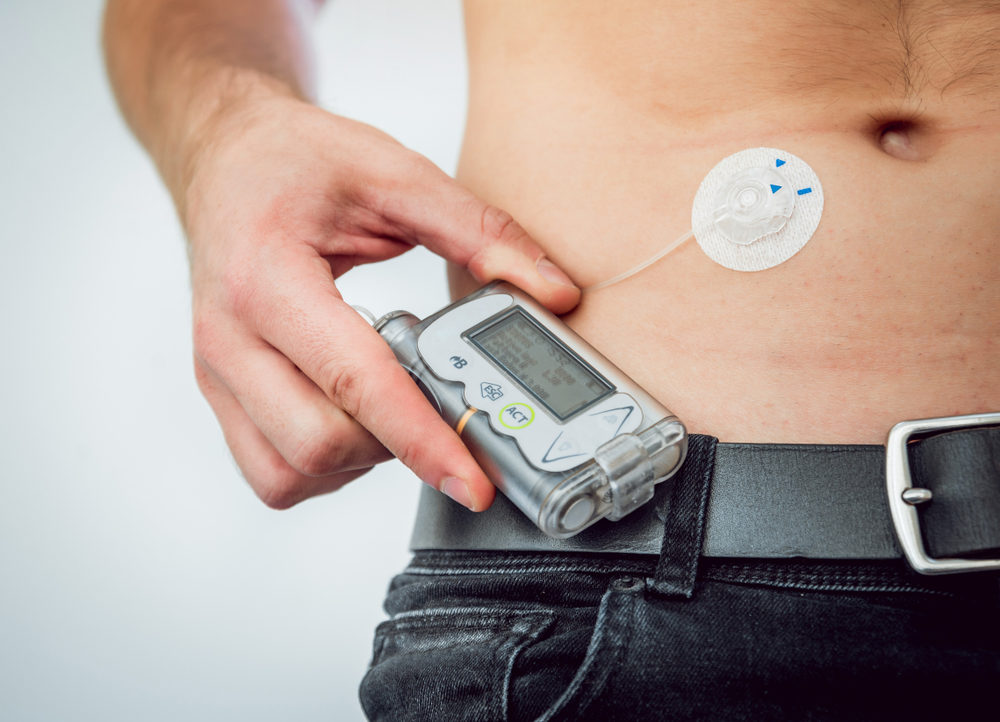
Amid concerns about continuing problems with infusion pumps, which may result in serious and potentially life-threatening medication errors, a group of experts has issued new guidelines that are designed to ensure the safe implementation of “smart” infusion pumps in healthcare settings.
The Institute for Safe Medication Practices (ISMP) released new smart infusion pump guidelines on February 11, focusing on key barriers to the safe and full implementation of the devices, including limitations on pump capabilities, alarm fatigue, persistent deficiencies related to library use and updates, availability of pumps, programming workflow, associated risks with secondary infusions, and pump data analysis.
The prominent non-profit organization, which oversees the healthcare community’s safe medication practices, held a national summit in 2018 to discuss medication errors and the smart infusion pump problems, which led to the development of these new guidelines.

Did You Know?
Millions of Philips CPAP Machines Recalled
Philips DreamStation, CPAP and BiPAP machines sold in recent years may pose a risk of cancer, lung damage and other injuries.
Learn MoreSmart infusion pumps were first used in hospitals 20 years ago. Since then, 80% of U.S. hospitals now use them as part of standard of care to reduce medication errors. Despite being one of the most ubiquitous devices in healthcare, the devices are not often fully integrated into the healthcare system.
The ISMP warns that many hospitals do not link smart infusion pumps with other technology to help prevent medication errors and ensure patient safety. For example, smart infusion pumps are still not linked to the bar-code medication systems used as one step in ensuring correct medication and dosing and are not linked to the patient electronic health record system.
Often pumps are made to operate in isolation from other electronic systems and require manual programming.
Smart Infusion Pump Guidelines
The guidelines focus on six key areas hospitals must focus on to ensure smart infusion pumps are implemented into the system effectively: specific error reduction strategies, infrastructure, drug libraries, continuous quality improvement data, clinical workflow, and interoperability with the electronic health record (EHR).
The guidelines indicate use of smart infusion pump technology should be an expected practice throughout the organization in every department, an expected part of the healthcare provider’s infrastructure.
Smart infusion pumps have the ability to detect and warn about possible medication errors, but hospitals are not fully using the tech and serious errors have continued, according to the ISMP. The group recommends hospitals establish a team to test the drug library and update it quarterly.
To focus on continuous quality improvement data, the hospital should provide dedicated time and resources for reviewing and analyzing pump data, at least on a quarterly basis, according to the recommendations.
The ISMP indicates the administration set should be installed on all infusion pumps to ensure clinical workflow and to not disrupt quality of care. Finally, the hospital must focus on establishing a team to guide and implement interoperability between the pump and the EHR.
The updated guidelines aim to help healthcare practitioners better use safety features of smart infusion pumps and ensure the pumps are fully integrated in technology used everyday in the healthcare setting.
The ISMP solicited feedback from users to identify safety gaps and conducted three practitioner surveys following the summit to better gauge successes, safety concerns, and barriers to optimization before establishing the guidelines.
“Infusion pump-related errors have frequently occurred due to a failure to engage the dose error-reduction system and the ease with which providers may select the wrong drug library entry or override serious alerts,” says ISMP Director of Consulting Services Michelle Mandrack. “ISMP has sought input from end users and key stakeholders to identify safety gaps and expand the compendium of expert-and evidence-based best practices available in this area to better protect patients.”
Get more articles like this sent directly to your inbox.
"*" indicates required fields




0 Comments