More Than 200 Duodenoscope Problems Reported to FDA Since October, But Number is Declining
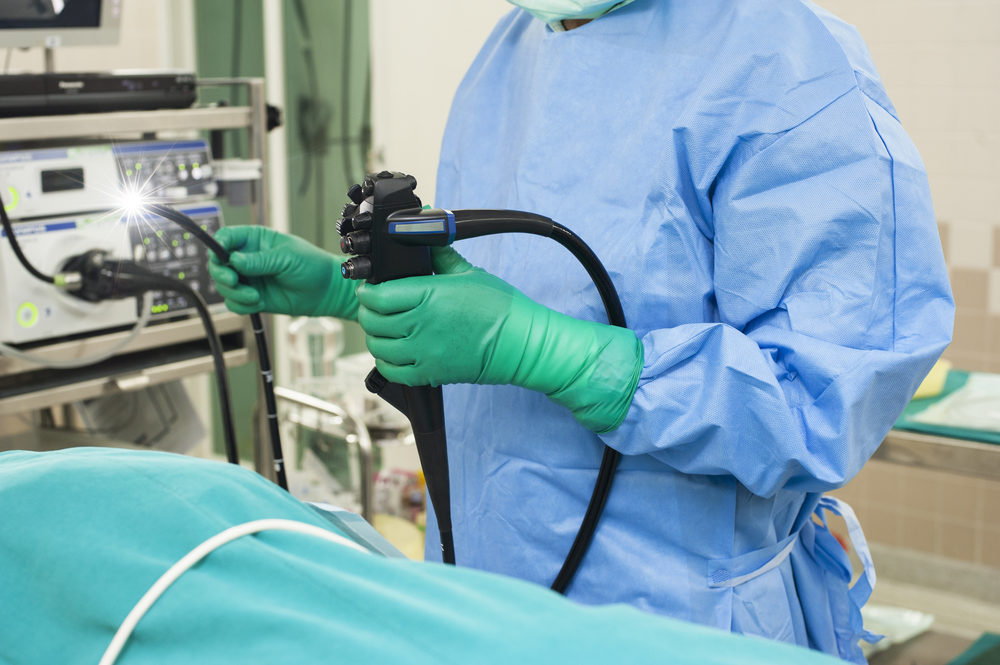
Federal regulators urge doctors and other healthcare professionals to closely follow instructions for sterilizing duodenoscopes, noting they have received more than 200 adverse event reports involving problems with the devices in the past six months, including dozens of cases of infections.
The FDA issued a safety communication on April 12, releasing new postmarket surveillance data on rates of contamination following the cleaning and reprocessing of duodenoscopes.
The data indicates there were 205 duodenoscope problems reported between October 15, 2018 and the end of March 2019, including 45 incidents of infections. The data also included 159 reports of device contamination. The FDA notes that in 2018, three deaths were linked to the use of duodenoscopes in the United States.

Did You Know?
Millions of Philips CPAP Machines Recalled
Philips DreamStation, CPAP and BiPAP machines sold in recent years may pose a risk of cancer, lung damage and other injuries.
Learn MoreDuodenoscopes are used during endoscopic retrograde cholangiopancreatography (ERCP) procedures, but difficulties cleaning device manufactured by several different companies have resulted in reports of serious hospital infection outbreaks, typically involving aggressive, antibiotic-resistant “superbugs”, which have caused a number of severe injuries and deaths.
The safety of the devices first emerged after a duodenoscope infection outbreak at UCLA’s Ronald Reagan Medical Center in February 2015, involving carbapenem-resistant enterobacteriaceae (CRE) infections that resulted in at least seven infections and two deaths. At least 200 other patients had to undergo testing after being placed at risk by duodenoscopes manufactured by Olympus Corp.
The infections were linked to problems with the “reprocessing” instructions provided by the manufacturer, which are used to clean the devices for use by another patient. FDA reviewers determined that the instructions sent out at the time were inadequate and that even if the recommended steps were followed to clean ERCP endoscopes, flaws in the design may allow them to become easily contaminated.
In October 2015, the FDA ordered Fujifilm, Olympus and Pentax, the three manufacturers of duodenoscopes in the U.S., to conduct postmarket surveillance studies of the effectiveness of the cleaning instructions. The studies parameters called for a contamination rate of no higher than 0.4%.
According to the latest update, 5.4% of samples tested positive for organisms of “high concern”, while 3.6% of samples tested positive for organisms of low and moderate concern.
Dr. Jeff Shuren, director of the FDA’s Center for Devices and Radiological Health, noted that while the safety of duodenoscopes do seem to be improving, these detection rates are far outside what the agency deems satisfactory.
“Let me be clear, the percent of contaminated samples based on these interim results shows that improvements are necessary and we are committed to taking additional steps to reduce infections and contamination even further,” he said in a separate statement. “The FDA previously instructed the manufacturers to conduct root cause analyses following the preliminary results announced last December to better understand these culturing results. These analyses are currently underway with an analysis of the newly collected samples, and final results are expected later in 2019.”
The FDA is currently consulting with the U.S. Centers for Disease Control and Prevention (CDC) to explore what additional steps can be taken to reduce contamination rates, Shuren announced.
Next month the FDA and CDC are holding a Healthcare Infection Control Practices Advisory Committee meeting to seek input from stakeholders on how to improve the safety of the devices.
The meeting is scheduled for May 16 and 17 at the CDC in Atlanta, Georgia.
Get more articles like this sent directly to your inbox.
"*" indicates required fields




0 Comments