Hip Replacements Often Used With No Evidence of Effectiveness: Study
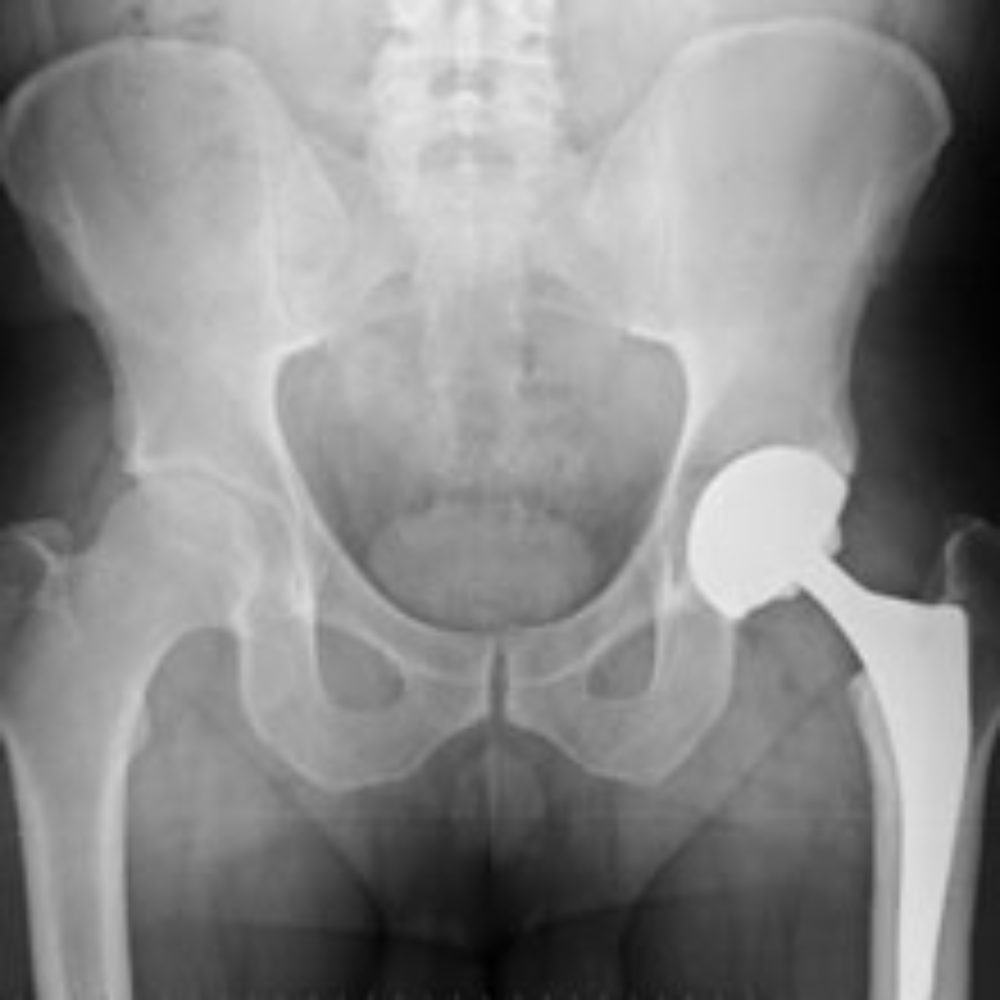
The findings of a new study suggest that nearly a quarter of all artificial hip implants used are not adequately tested for safety and effectiveness.
Researchers from the U.K. found that many hip replacement systems are placed on the market with no clinical studies completed to confirm whether they actually work, and there is insufficient data to examine the potential risks faced by patients.
The study was published last month in the British Medical Journal, coming after several years of high profile hip replacement recalls and product liability lawsuits filed over implants that were found to be dangerous and defective long after they were introduced to the market.

Learn More About
Lawsuits are being reviewed for several different dangerous and defective hip replacement systems.
Learn More About this Lawsuit SEE IF YOU QUALIFY FOR COMPENSATIONMany of the problems discovered in recent years were identified through hip implant registry systems, which have been put in place in the U.K., Australia and other countries to track all artificial implants; keeping tabs on which ones fail and why.
This latest study compiled data from the 9th annual report from the National Joint Registry of England and Wales (NJR). Researchers found that “24% of all hip replacement implants available to surgeons in the U.K. have no evidence for their clinical effectiveness.” Of the 10,617 hip implants and components implanted in U.K. patients in 2011, 8% of those procedures were performed with untested parts. The study contains a list of all of the untested devices.
Hip Implants and Medical Devices Under Scrutiny
“Medical device regulation has been the subject of recent debate,” the researchers stated. “Both professional and public confidence in the system is at a low point. This is particularly true in orthopaedics, where the premature failure of some metal-on-metal hip replacements has added considerably to the global burden of hip revision.”
Perhaps the highest profile metal-on-metal hip replacement system failure has been the DePuy ASR inmplant. A DePuy ASR hip recall was issued in August 2010, after a review of the NJR found failure rates of 12-13%. Later registry data suggested that the failure rates may actually be as high as 30%.
In the wake of the recall, thousands of DePuy ASR hip lawsuits were filed by patients who had to undergo revision surgery. DePuy Orthopaedics, a division of Johnson & Johnson, has agreed to a DePuy ASR settlement that is likely to cost at least $2.4 billion, and could top $4 billion. However, the settlement will only go into effect if virtually all DePuy ASR lawsuit plaintiffs join the settlement agreement.
Questions about the safety of the metal-on-metal hip design has led to other litigation over similar systems, including the DePuy Pinnacle, Biomet Magnum, and the Wright Medical Conserve Cup .
According to allegations raised in complaints brought against the makers of metal-on-metal hip systems, the design is defective and unreasonably dangerous, as it results in the release of metal debris into the body as the metal parts rub against each other, causing metal blood poisoning, known as metallosis, tumors, and catastrophic failure.
Concerns have also emerged in recent years about another type of new hip design, known as modular hip replacement systems. Unlike traditional hip implants, which feature a single femoral component, modular hip designs feature two pieces that fit inside each other, allowing the doctor to adjust the length of the component based on the patient. However, problems have emerged where the modular implants may fracture or cause premature failure.
One of the first modular hip implants introduced was the Wright Profemur, which has been linked to reports of fractures at the femoral neck. There are a number of Wright Profemur hip lawsuits pending in courts throughout the United States, and subsequent changes have been made to the design of the system to improve the strength. However, these changes came after thousands of individuals received the original implant.
Another modular hip implant, known as the Stryker Rejuvenate, has also been linked to problems where the components were found to fret, corrode and fail. While hip replacements are typically expected to last 15 to 20 years, a Stryker Rejuvenate recall was issued only two years after the design was introduced, amid reports of high failure rates. The manufacturer now faces more than 1,000 Stryker Rejuvenate hip lawsuits, and the number of complaints continues to grow as more-and-more patients experience problems with the implant.
In the United States, the FDA has faced criticism over the fast-track approval given to many artificial hip systems, under the agency’s controversial 510k approval program. This process allows medical device manufacturers to introduce new products without substantial clinical trials if they can establish that the device is substantially similar to an existing approved device. However, critics say that manufacturers have abused the system by fielding virtually new medical devices under the system; claiming they are identical to existing devices on one hand and heralding their new improvements and significant differences on the other.
“The evidence presented in this study relates to prostheses implanted in the U.K. However, we believe the results of this study can be applied to other healthcare settings, given that most of the prostheses in our systematic review are available in most other developed countries, in Europe, Australasia, and the United States,” the researchers concluded. “This study shows that the need still exists for an improved and more rigorous approach to regulation of devices to avoid devices with no available evidence being used in a widespread and uncontrolled manner.”
Get more articles like this sent directly to your inbox.
"*" indicates required fields



0 Comments