TAVR Valve Size May Play Role In Chances Of Survival: Study
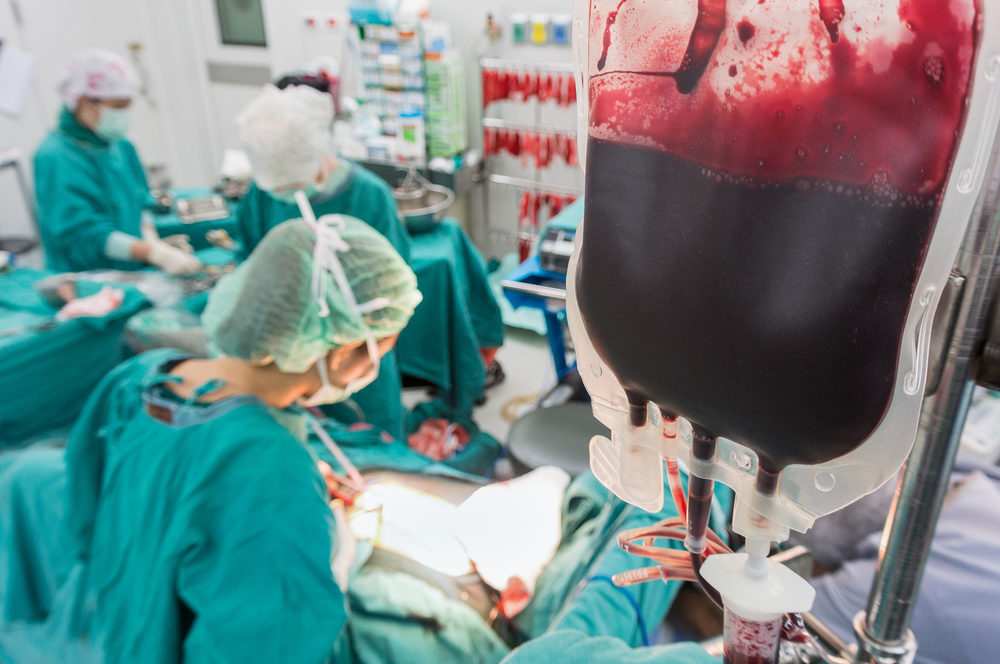
The type and size of a failed transcatheter valve could play a crucial role in the risk of a patient dying or needing a second surgery later, according to the findings of a new study.
University of Washington Medical Center researchers report that patients who underwent a valve-in-valve (ViV) surgery to repair a previous, failed transcatheter aortic valve replacement (TAVR) had lower survival rates and were more likely to need another surgery depending on certain factors, such as the size of the valve.
TAVR is a type of heart procedure that allows the surgeon to replace the heart valve by threading it through an artery in the leg instead of via open chest surgery. It places the valve over the damaged aortic valve in a less invasive procedure.

Did You Know?
AT&T Data Breach Impacts Millions of Customers
More than 73 million customers of AT&T may have had their names, addresses, phone numbers, Social Security numbers and other information released on the dark web due to a massive AT&T data breach. Lawsuits are being pursued to obtain financial compensation.
Learn MoreInitially, TAVR was approved only in high risk patients who were frail or couldn’t undergo open heart surgery because the procedure carried such high risks. More so, the durability of the heart valves was untested for use in younger patients who would outlive the devices that were designed to last 10 years, not 30 or more years.
In this latest study, researchers conducted an analysis of the valve-in-valve international data VIVID registry. They identified more than 1,000 patients with bioprosthetic valve failure who received ViV procedures before 2014, mostly Medtronic self-expanding valves or Edwards balloon-expandable valves.
According to the findings, patients more likely to have a failed valve and need surgical intervention included those whose surgical valves had a smaller internal diameter, who were older, had reduced left ventricular ejection fraction, chronic kidney disease, whose surgeons used a non-transfemoral access during surgery, and who had diabetes.
Those patients were also more likely to suffer early death.
The size of the original failed bioprosthesis and the type of transcatheter valve implanted were linked to estimated survival at 8 years among the more than 1,000 ViV transcatheter aortic valve replacement patients studied.
The researchers looked at survival rates over eight years and found a connection to the size and type of valve implanted. Smaller bioprosthesis valves appeared to have lower survival rates.
For example, the survival rate for Edwards balloon-expandable valves with an internal diameter of 20mm or less was 26.6%, compared to a 43.6% survival rate for large Medtronic self-expanding valves.
Second surgery rates were 6% for patients with balloon expandable valves compared to 2% for patients with self-expanding valves.
Surgical reintervention was also more common with pre-existing severe patient-prosthesis mismatch. Patients who were severely mismatched had a reintervention rate of 12.5% compared to a 3% rate for those who were not mismatched.
Patients who were younger, had balloon-expandable valves, and bad valve positions, or pre-existing severe PPM were more likely to need re-interventions as well.
Researchers indicated the findings emphasize the importance of good preoperative planning by surgeons. This can include using CT scans to select the best valve, size and placement for the patient instead of using a cookie-cutter approach.
They indicated there are two things surgeons can do to optimize hemodynamics before the first valve surgery. First, place the transcatheter valves as high as possible. Second, fracture the surgical prosthesis to allow the TAVR valve to expand fully, preventing some future complications and reducing the need for another surgery.
The findings were presented during the PCR e-Course Conference held virtually in lieu of the cancelled EuroPCR meeting. The study is considered preliminary until published in a peer-reviewed journal.
Want a weekly update on top lawsuits, recalls & warnings?
"*" indicates required fields





0 Comments